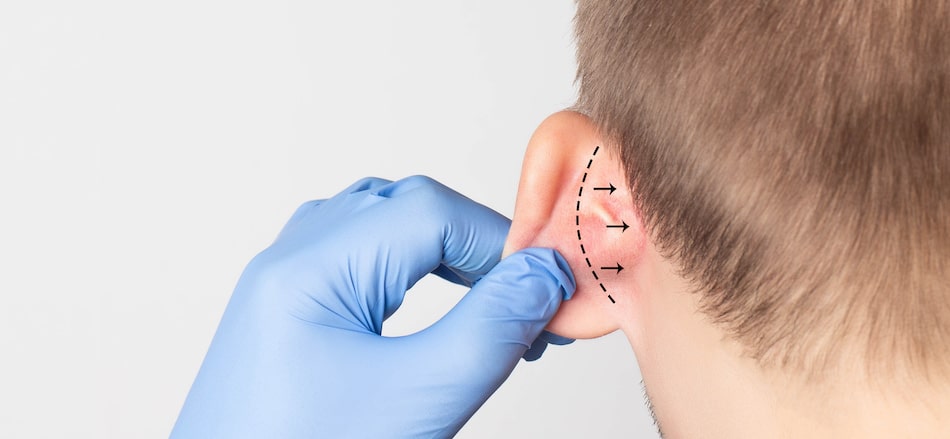
Otoplasty is a very popular cosmetic surgery procedure as the ears are one of the most prominent features on the human body. If a person is born with ears that are deformed or ears that have a prominent look because they stick out in a noticeable manner from the head, the patient might turn to otoplasty to make a change in the size or shape of the ears. There have been some recent developments in the field of otoplasty that show an opportunity for patients to enjoy a new ear reconstruction method in the future as covered in the informative article below and by Cosmetic Town TV:
According to numbers from the National Birth Defects Prevention Network, one in every 8000-10,000 births that occur in the United States involve one of two congenital malformations that can happen with the ear:
When both of these conditions occur, the child usually experiences partial deafness as well since the ear canal or ear drum is not properly shaped. Partial deafness occurs because lack of a properly shaped ear drum or ear canal means there is no way to capture and relay sound waves.
 As recently reported in Science Daily, two novel tools that were developed by a resident at John Hopkins Medicine, as well as a former resident, might be able to make the task of replacing an ear easier than was required in the past. They hope the often difficult surgery to create a replacement ear through the use of the rib cartilage of a patient can be performed quicker and more accurately and not waste any potentially valuable tissue. In addition, there is a hope that this new technique can provide patients with a “custom fit” for the newly created ear.
As recently reported in Science Daily, two novel tools that were developed by a resident at John Hopkins Medicine, as well as a former resident, might be able to make the task of replacing an ear easier than was required in the past. They hope the often difficult surgery to create a replacement ear through the use of the rib cartilage of a patient can be performed quicker and more accurately and not waste any potentially valuable tissue. In addition, there is a hope that this new technique can provide patients with a “custom fit” for the newly created ear.
Angelo Alberto Leto Barone, M.D., a former resident in plastic and reconstructive surgery at John Hopkins School of Medicine, said, “Although ear reconstruction surgery for repairing microtia and anotia in both pediatric and adult cases has been practiced for a number of years, it still is a demanding procedure for both the patient and the surgeon. Barone, who is now a craniofacial and pediatric plastic surgeon at Nemours Children’s Health in Orlando, Florida, added, “What makes it really difficult is that to construct a suitable ear requires a bit of artistic skill.”
Barone and Anirudh Arun, M.D., a John Hopkins interventional and diagnostic radiology surgery resident, invented two assistive devices by using 3D manufacturing. The first device is a carving tool that works to slice rib cartilage from the body of the patient. The rib cartilage can be sliced to any desired level of thickness while also minimizing any tissue waste. The second device uses steel blades that are shaped in patterns fashioned from the normal ear of a patient. This more “cookie cutter” approach produces cartilage pieces that are brought together during the surgery to form the new ear.
Arun said, “The cartilage-slicing device basically doubles the amount of cartilage tissue available for surgery, meaning that less has to be harvested to safely produce the entire ear. We only need two and a half ribs instead of the traditional four from prior techniques – less waste and less discomfort for the patient.” When the cartilage slices are placed into the cutter, they are trimmed in a precise manner to form the components of the new ear in a matter of minutes instead of the multiple hours that are needed when using a scalpel.
Barone shared that the process is quicker and that “the template eliminates the cartilage damage that often accompanies the sculpting done in previous reconstruction methods. This makes our system highly reproducible, user friendly, time efficient, and cost effective. Best of all, it consistently yields a natural-looking ear that helps children avoid being teased or bullied, and enables adults to do things other take for granted, like wearing glasses.”
Barone and Arun recently tested their assistive devices during an in-human trial which was surgery on a teenage patient. They shared the successful results in a research letter published in Facial Plastic Surgery & Aesthetic Medicine.
Arun noted that their system performed exactly as it was designed and, when compared to more traditional ear reconstruction techniques, they used less cartilage while also following a “standardized procedure for constructing the ear framework and decreased the operating time required for that construction.”
The duo are now exploring additional uses for their devices such as adapting them to build structures that can replace other facial features, such as eyelids and nose cartilage, that were missing at birth, malformed, or damaged by some form of trauma or disfiguring event.
They have also been approved for a patent for their two-device system.
Additional authors on the research letter include Thomas Harris, Jordan Steinberg, Neha Datta, and Richard Redett. Plus, George Samaha at the University of Miam School of Medicine was also a contributing author.
- MA