Breast augmentation is the second most popular surgical cosmetic procedure - after liposuction - performed in the United States and is utilized to increase the breast size. The majority of breast augmentation cases are performed using implants made from either saline or silicone; a much smaller percentage of cases is performed using fat transfer. An incision is necessary when an implant is used for breast augmentation, and every incision results in a scar.
Scars form as the body’s attempt to heal following an injury. An incision from surgical procedure is considered an injury, albeit a controlled one, so scar develops in the site where the cut is made. Scars respond to external pressure like tension. Tension pertains to forces that tug the edges of tissue that are trying to heal together. If the skin in the area of the incision is under tension, then the scar will respond by becoming thicker and harder in an effort to cleave together.
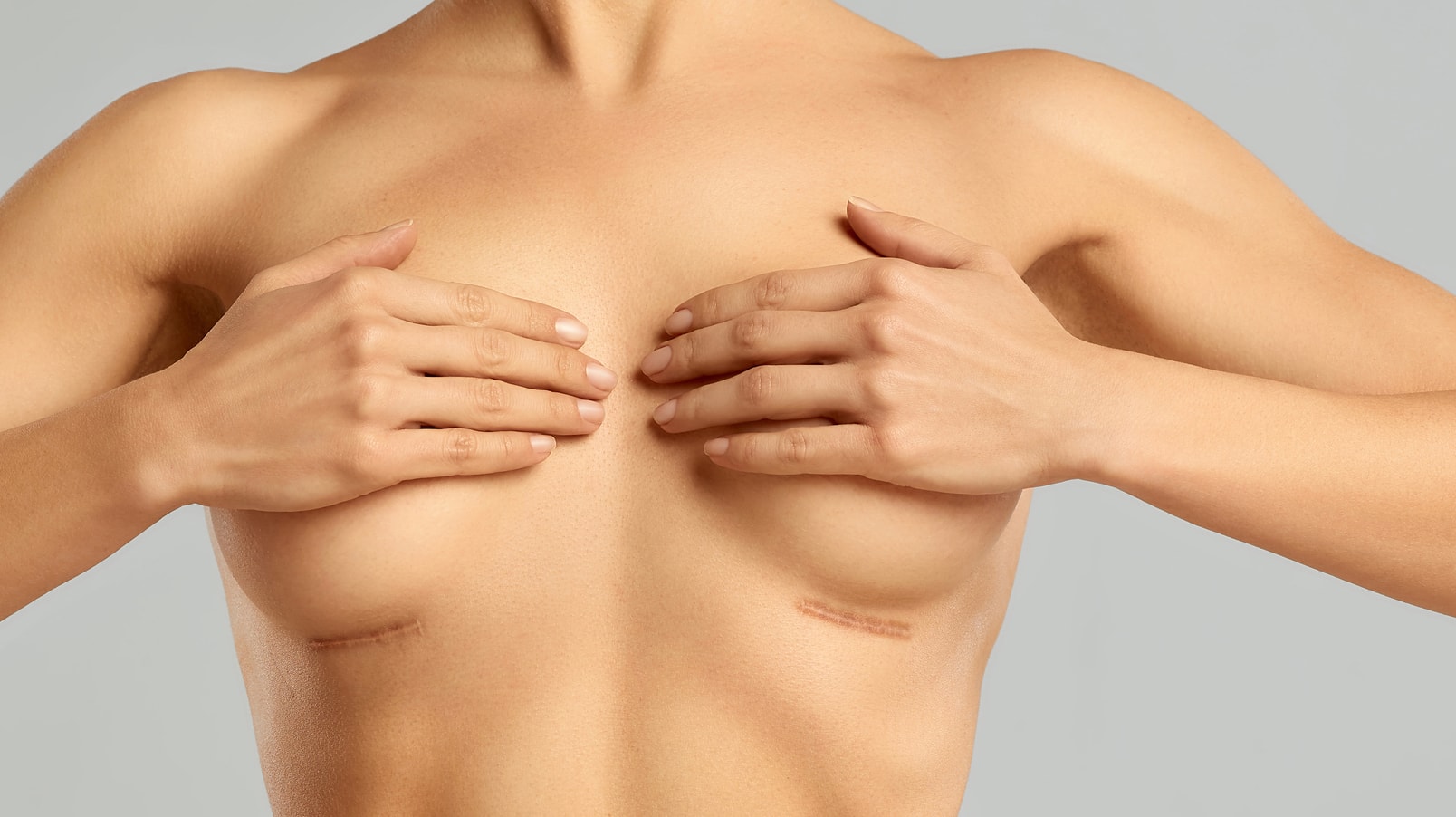
Any procedure that involves an incision results in a scar. There are various types of incisions used to perform breast augmentation: the inframammary fold incision (IMF), the periareolar incision, and the axillary incision. The inframammary fold incision is the most common among the three. In this type, the incision is made under the breast in the crease where the breast meets the chest wall. This area has the lowest counts of bacteria compared to the others, a factor that carries lower rates of capsular contracture and wound infection. It is also generally accepted that this approach affords the best visualization of the pocket where the implant goes, thus it is easier to control bleeding and the shape of the pocket.
The periareolar approach entails incising the border of the areola. This works well to camouflage the incision and is a very reasonable choice for breast augmentation. Compared to inframammary incision, however, the periareolar approach entails a higher risk of implant infection as the nipple is impossible to sterilize give the presence of ducts in the area. An axillary approach entails creating an incision in the armpit. While it saves the breast from an incision, the scar can be visible when the patient raises her arms, it is harder to visualize the breast pocket, and, again, compared to the IMF incision, there is a higher risk of infection in this area given the increased presence of bacteria.
There is no way to completely avoid scarring, but there are ways to minimize it. One is by wearing a supportive garment at all times to alleviate tension. It may also be beneficial to limit the size of implants in order to reduce the weight (i.e. tension) on the scar.
Genetics is another key factor determining the appearance of a scar. If the patient has thicker collagen or is dark-skinned, there is an increased likelihood of hypertrophic or keloid scars compared to lighter-complexioned people. Hypertrophic scars are puffy and thickened but stay in the boundary of the original incision. Keloid scars are puffy and thickened but extend beyond the original boundary. They may both be managed with a variety of modalities including steroid injections, pressure dressings, and silicone sheeting; however, no modality is 100% effective, thus hypertrophic and keloid scars are a difficult problem.
Infection can also bring worsen the ultimate appearance of scars. Inflammation of the tissues caused by infection leads to the breakdown of healthy tissues, resulting to wider and thicker scars. If infection is prevented, then there will be less inflammation and an increased likelihood that the scar will heal well.
Sun exposure (ultraviolet radiation) also tends to make scars whiter and more obvious. Weight-gain and aging have their effects on scars. Weight gain increases the tension on a healing scar. Even after the scar has actually healed, there may still be some degree of stretch. Aging, on the other hand, tends to weaken collagen. Collagen makes the skin more elastic, and it also plays a role in the body’s ability to heal itself. Smoking also weakens collagen and severely hinders an incision’s ability to heal.
There are many treatments to improve the appearance of scarring. Silicone products and sheeting help soften and flatten scars. Laser resurfacing is another option that may improve the texture and decrease the redness of scars. Finally, if ancillary treatments fail, surgical excision is an option. As scars take time to mature, surgical scar revision is not typically done for a year after the initial incision. Surgical excision itself carries complications including pain, bleeding, swelling, infection and the risk of recurrent poor scarring.
There will always be a line in the skin, however faint, from breast augmentation. There are, however, ways to minimize scarring. It is important to consult with a board-certified plastic surgeon for breast augmentation as they may assess your risk factors for poor scarring, offer options for the approach, perform a meticulous surgery to minimize those risk factors, and monitor you post operatively.
Written by Cosmetic Town Editorial Team - AA
Based on an exclusive interview with Whitney Burrell, MD in Torrance, CA